In heart failure with a low cardiac output state, activation of the RAAS serves as a compensatory mechanism to maintain cardiac output. Reduced renal blood flow and sodium delivery to the distal tubule leads to renin release, which is exacerbated further by increased sympathetic tone.
How does renin-angiotensin-aldosterone system affect heart failure?
Activity of the renin-angiotensin-aldosterone system (RAAS) is increased in patients with heart failure, and its maladaptive mechanisms may lead to adverse effects such as cardiac remodelling and sympathetic activation. Elevated renin activity has been demonstrated in patients with dilated cardiomyopathy.
Why does heart failure increase renin?
Increases in renin, mediated by a decreased stretch of the glomerular afferent arteriole, reduce delivery of chloride to the macula densa and increase beta1-adrenergic activity as a response to decreased cardiac output.
What are the consequences of renin angiotensin system activation?
In these local systems, activation of angiotensin II results in harmful effects and target-organ damage that extend beyond vascular and renal hemodynamics to direct tissue actions, including tissue remodeling, endothelial dysfunction, and fibrosis.How does the renin angiotensin system Ras activation contribute to increased afterload and heart failure?
The renin-angiotensin system (RAS) mediates many of these compensatory responses. Increased angiotensin can result in net vasoconstriction and increase afterload. In addition, it contributes to the avid sodium retention that occurs in patients with CHF.
Which is an end result of the renin angiotensin system?
Activation of the renin–angiotensin–aldosterone system (RAAS) results in vasoconstriction, muscular (vascular and cardiac) hypertrophy and fibrosis. Established arterial stiffness and cardiac dysfunction are key factors contributing to subsequent cardiovascular and renal complications.
How does activation of the renin angiotensin mechanism affect blood pressure?
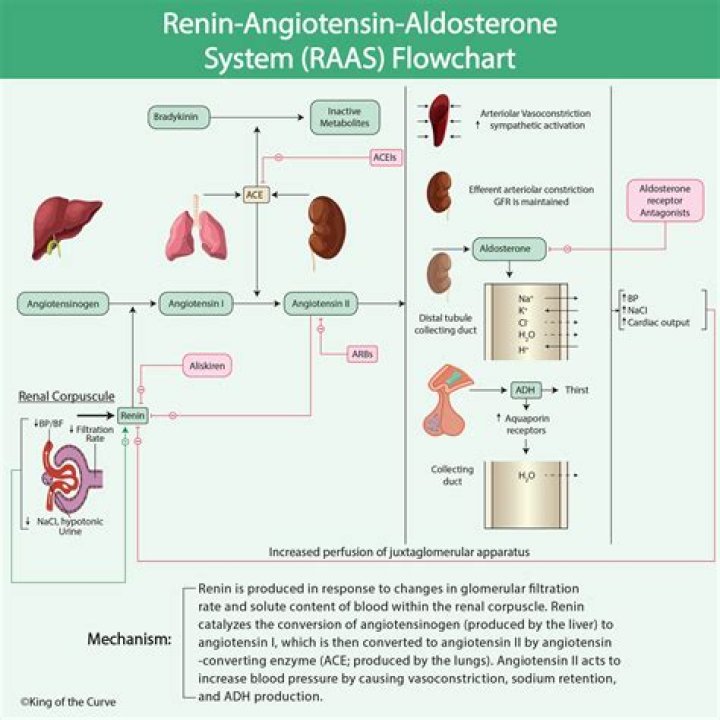
Renin converts angiotensinogen, which is produced in the liver, to the hormone angiotensin I. An enzyme known as ACE or angiotensin-converting enzyme found in the lungs metabolizes angiotensin I into angiotensin II. Angiotensin II causes blood vessels to constrict and blood pressure to increase.
How does angiotensin II affect blood pressure?
Angiotensin II receptor blockers help relax your veins and arteries to lower your blood pressure and make it easier for your heart to pump blood. Angiotensin is a chemical in your body that narrows your blood vessels. This narrowing can increase your blood pressure and force your heart to work harder.What effect does angiotensin II have on the body?
Angiotensin II (Ang II) raises blood pressure (BP) by a number of actions, the most important ones being vasoconstriction, sympathetic nervous stimulation, increased aldosterone biosynthesis and renal actions.
How does angiotensin affect the cardiovascular system?Angiotensin, specifically angiotensin II, binds to many receptors in the body to affect several systems. It can increase blood pressure by constricting the blood vessels. It can also trigger thirst or the desire for salt.
Article first time published onWhy is the renin angiotensin system important?
The renin-angiotensin-aldosterone system (RAAS) is one of the most important hormonal mechanisms in controlling hemodynamic stability by regulating blood pressure, fluid volume, and sodium-potassium balance.
How is the renin angiotensin aldosterone system activated?
Typically, RAAS is activated when there is a drop in blood pressure (reduced blood volume) to increase water and electrolyte reabsorption in the kidney; which compensates for the drop in blood volume, thus increasing blood pressure.
What effect does the renin-angiotensin-aldosterone system have on stroke volume?
The RAAS functions to elevate blood volume and arterial tone in a prolonged manner. It does this by increasing sodium reabsorption, water reabsorption, and vascular tone.
What is the main function of the renin-angiotensin-aldosterone system RAAS?
The renin-angiotensin-aldosterone system (RAAS) is a well known regulator of blood pressure (BP) and determinant of target-organ damage. It controls fluid and electrolyte balance through coordinated effects on the heart, blood vessels, and Kidneys.
How does the RAAS system contribute to Oedema in heart failure?
Sustained sympathetic stimulation activates the renin-angiotensin-aldosterone system and other neurohormones, leading to increased venous and arterial tone (and greater preload and afterload respectively), increased plasma noradrenaline concentrations, progressive retention of salt and water, and oedema.
What effect would his low blood pressure have on the renin-angiotensin aldosterone system?
In addition, low blood pressure can stimulate the sympathetic nervous system to increase renin production, which results in increased conversion of angiotensinogen to angiotensin I, and so the cycle continues.
What is the role of renin in regulation of blood pressure?
When blood pressure falls (for systolic, to 100 mm Hg or lower), the kidneys release the enzyme renin into the bloodstream. Renin splits angiotensinogen, a large protein that circulates in the bloodstream, into pieces.
Does renin decrease blood pressure?
Renin by itself does not really affect blood pressure. Instead, it floats around and converts angiotensinogen into angiotensin I. Angiotensinogen is a molecule that is primarily produced by the liver and circulates throughout the bloodstream. It is not able to alter the blood pressure as a precursor molecule.
Which one of the following are the main functions of renin and angiotensin II?
The Renin-Angiotensin-Aldosterone System (RAAS) is a hormone system within the body that is essential for the regulation of blood pressure and fluid balance. The system is mainly comprised of the three hormones renin, angiotensin II and aldosterone. Primarily it is regulated by the rate of renal blood flow.
How would decreasing the action of angiotensin II reduce blood pressure from a kidney function standpoint?
Presumably, blood pressure reduction by Ang II blockade stimulates sympathetic nerve activity, which prevents afferent arteriolar vasodilation, allowing glomerular pressure to fall1).
What are some effects of angiotensin II quizlet?
Angiotensin II causes increased sympathetic nervous system activity, which increases blood pressure. Angiotensin II causes cardiac remodeling, which increases blood pressure. Angiotensin II increases the reabsorption of sodium, which increases blood pressure.
How would high levels of angiotensin II affect hypertension?
The renin-angiotensin system (RAS) plays an important role in the regulation of blood pressure. Angiotensin II is the principal effector hormone in the RAS, causing vasoconstriction and increased sodium and water retention, leading to increased blood pressure.
What are the side effects of angiotensin II receptor blockers?
- headache.
- fainting.
- dizziness.
- fatigue.
- respiratory symptoms.
- vomiting and diarrhea.
- back pain.
- leg swelling.
What are the 3 stimuli that cause the release of renin?
Mechanism of Action. Increased renin release from the juxtaglomerular cells is caused by several conditions: reduction in renal blood flow from heart failure, blood loss, hypotension or ischemia of the kidneys, sodium diuresis (excessive sodium loss in urine), and beta-adrenergic stimulation.
Where does renin angiotensin system work?
The renin-angiotensin-aldosterone system is a series of reactions designed to help regulate blood pressure. When blood pressure falls (for systolic, to 100 mm Hg or lower), the kidneys release the enzyme renin into the bloodstream.
How does angiotensin 2 affect the heart?
Angiotensin (Ang) II, through the activation of specific Ang II receptors, regulates cardiac contractility, cell communication, and impulse propagation. In addition, Ang II is involved in cardiac remodeling, growth, and apoptosis.
Does angiotensin increase heart rate?
Angiotensin increases blood pressure without decreasing heart rate because it resets the baroreflex control of heart rate to a higher pressure.
What is the role of renin in the secretion of aldosterone quizlet?
It stimulates the synthesis of new sodium and potassium CHANNELS in the apical membrane. The renin-angiotensin-aldosterone system is a long-term endocrine pathway that regulates extracellular fluid volumes including blood plasma, lymph and interstitial fluid. RAAS also regulates arterial vasoconstriction.
Does aldosterone increase cardiac output?
Therefore, our experiments show that aldosterone induces a primary increase in cardiac output followed by a secondary vasoconstriction, which is consistent with the classical transient haemodynamic effects of volume-loading hypertension.
What effect would the change in MAP due to heart failure have on RAAS and ADH?
As a result of left ventricle heart failure, the left ventricle of the heart muscle has a reduced ability to pump; this causes MAP to decrease and trigger activation of the RAAS and release of ADH.
How does the renin-angiotensin-aldosterone system affect glomerular filtration rate?
To do this, angiotensin II constricts efferent arterioles, which forces blood to build up in the glomerulus, increasing glomerular pressure. The glomerular filtration rate (GFR) is thus maintained, and blood filtration can continue despite lowered overall kidney blood flow.