The trendelenburg gait
What does Trendelenburg sign indicate?
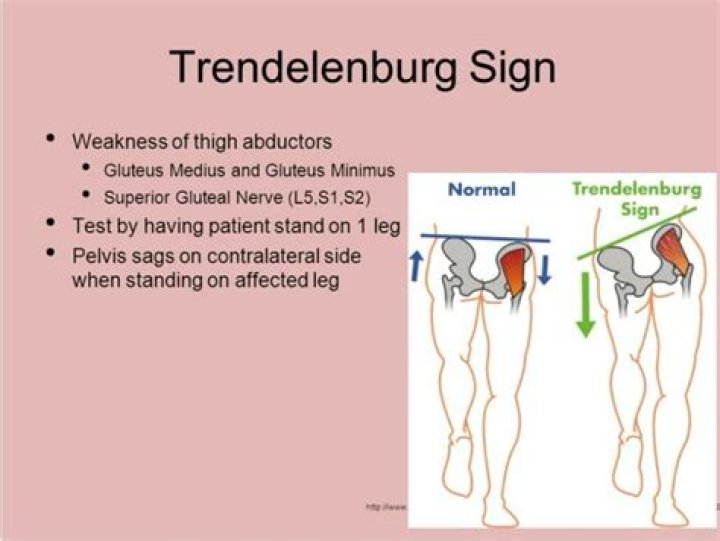
Definition/Introduction Trendelenburg sign is a physical examination finding seen when assessing for any dysfunction of the hip. A positive Trendelenburg sign usually indicates weakness in the hip abductor muscles consisting of the gluteus medius and gluteus minimus.
What nerve causes Trendelenburg gait?
Many times, the muscle weakness that causes the Trendelenburg gait starts with damage to the superior gluteal nerve, which originates in the pelvis and ends in the gluteus minimus muscle. When this nerve is damaged, it’s hard for the affected side to support the weight of the body.
What causes a positive Trendelenburg test?
A positive Trendelenburg sign usually indicates weakness in the hip abductor muscles: gluteus medius and gluteus minimus. These findings can be associated with various hip abnormalities such as congenital hip dislocation, rheumatic arthritis, osteoarthritis.What happens in Trendelenburg gait?
The main symptom of Trendelenburg gait can be seen when one leg swings forward and the hip drops down and moves outward. This is because the hip abductor of the other leg is too weak to support your weight. You may lean back or to the side slightly as you walk to maintain your balance.
What Is Reverse Trendelenburg?
The Reverse Trendelenburg position is a position in which patients’ hip and knee are not flexed but the head and chest are elevated at 30° than the abdomen and legs.
How do I fix Trendelenburg?
Trendelenburg gait by itself wears the hip joint, and appropriate treatment is essential. Physical therapy is the mainstay treatment for gluteus medius and minimus weakness. Physical therapy involves strengthening the weakened hip abductor muscles.
What is the Trendelenburg test evaluating?
The Trendelenburg test is used to evaluate for weak or injured gluteus medius and minimus muscles. It begins with the patient in a neutral stance. The physician is seated behind the patient with his or her hands placed behind the patient’s hips with the thumbs resting on the posterior superior iliac spine.Why are my hip abductors so weak?
Underuse of the muscles or sitting down for extended periods can cause weak hip flexors. Conditions such as and osteoarthritis can also cause weakness in this muscle group.
Why is it called Trendelenburg gait?Trendelenburg gaitOther namesGluteus medius lurchSpecialtyNeurology
Article first time published onWhat is a hemiplegic gait?
Hemiplegic gait (circumduction or spastic gait): gait in which the leg is held stiffly and abducted with each step and swung around to the ground in front, forming a semicircle.
How do you stop waddling?
- Canes and walkers for balance.
- Physical therapy to help with strength, balance, and flexibility.
- Fall prevention measures.
- Leg braces or splints to help with foot alignment.
- Medicine.
- Surgery or prostheses.
What does Trendelenburg gait look like?
A trendelenburg gait is characterized by trunk shift over the affected hip during stance and away during the swing phase of gait and it is best visualized from behind or in front of the patient. During gait, the pelvis tilts downwards instead of upwards on the non-weight bearing extremity.
Does Trendelenburg gait cause knee pain?
Trendelenburg gait, otherwise referred to as a hip drop or trunk lean with walking are all compensatory movement patterns that may lead to back pain, hip pain, knee pain, or SI joint pain over time.
What is Trendelenburg lurch?
The Trendelenburg gait pattern (or gluteus medius lurch) is an abnormal gait caused by weakness of the abductor muscles* of the lower limb, gluteus medius and gluteus minimus which are supplied by the superior gluteal nerve.
Is pelvic tilt curable?
It’s possible to correct a posterior pelvic tilt with exercise. Learn five exercises you can do to help create strong leg and abdominal muscles to improve your posture.
What is a pelvic drop?
The term “pelvic drop” (also commonly referred to as hip drop) identifies moments when your pelvis lacks proper leveling, causing one side of your hip to drop lower than the other.
When should I stop Trendelenburg?
The Trendelenburg position should be avoided as a treatment of acute hypotension/shock until definitive research with larger sample sizes is conducted that support its use as safe and effective.
Does Trendelenburg increase cardiac output?
Placing the anaesthetized patients scheduled for CABG surgery in the Trendelenburg position resulted in a significant increase in cardiac output and mean arterial pressure and a non- significant decrease in heart rate.
Does Trendelenburg increase blood pressure?
However, researchers found that the use of Trendelenburg does not improve blood pressure and shock and instead, could have detrimental effects on specific patient populations.
How do you fix weak abductors?
Often used in both the therapy settings and among bodybuilders and weightlifters, these exercises help strengthen important muscles needed for stabilization and injury prevention. Exercises you can do to improve hip abductor strength include lying side leg lifts, clamshells, and banded side steps or squats.
How do you know if an abductor is weak?
When a client is walking on their right leg in the stance phase of the gait cycle and their left hip drops down, this indicates a weakness in the right hip abductors. If hip abductors are weak on both sides, it results in a waddling gait, which is reminiscent of the strut of a Vegas showgirl.
How do you know if you have a weak adductor?
The amount of strength noted should be equal. Squats can also be a telltale sign of hip adductor weakness, says Laudner: “If your knees point outward during a squat, then there could be an imbalance of hip strength with your hip adductors being weaker than the reciprocal hip muscles (hip abductors).”
What causes a dropped hip?
Hip drop is seen when someone is standing on one leg, and their pelvis tilts downwards towards the leg that is held in the air. Hip drop occurs when there is a weakness in our hip abductor muscles, most commonly the gluteus medius. When this muscle is strong, it keeps the pelvis level when standing on one leg.
How do you strengthen your pelvis?
To strengthen your pelvic floor muscles, sit comfortably and squeeze the muscles 10 to 15 times. Do not hold your breath or tighten your stomach, bottom or thigh muscles at the same time. When you get used to doing pelvic floor exercises, you can try holding each squeeze for a few seconds.
How can I adjust my pelvis at home?
- Lie on the floor, face upward, with knees bent.
- Squeeze the abdominal (stomach) muscles, so that the back is flat against the floor. Bend the pelvis slightly upward.
- Hold this position for up to 10 seconds.
- Repeat for five sets of 10 repetitions.
What is Trendelenburg test for varicose veins?
The Trendelenburg Test or Brodie–Trendelenburg test is a test which can be carried out as part of a physical examination to determine the competency of the valves in the superficial and deep veins of the legs in patients with varicose veins.
How do you strengthen your abductors?
- Stand on your right foot with your knee slightly bent. Hold a dumbbell in your left hand.
- Maintain a neutral spine as you hinge forward to bring your torso parallel to the floor. Lift your left leg.
- Come back up to standing. Lower your left leg.
- Do 2–3 sets of 8–15 repetitions on each side.
How do I fix my running gait?
- Make sure you have appropriate running shoes and change out your shoes often.
- Gradually increase the number of miles you run each week.
- Mix up running days with cross training, such as cycling or swimming.
- Warm up before you run and stretch after.
- Run with proper form.
How do you fix hemiplegic gait?
A common problem in hemiparetic gait, is the spastic inversion of the foot. If spasticity is not severe, an ankle-foot orthosis (AFO) is the appropriate technical aid. In other cases, botulinum toxin injection into spastic leg muscles has been successfully used to improve gait functions.
Can hemiplegia be cured?
Hemiplegia is a permanent condition and there’s no cure at this time. It’s known as a non-progressive disease because the symptoms don’t get worse over time. A person with hemiplegia who undergoes an effective treatment program may be able to improve the symptoms of their hemiplegia over time.