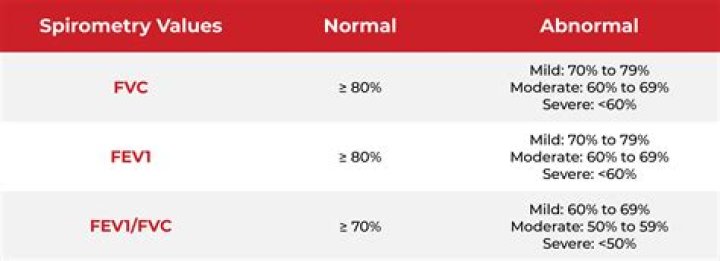
A lower-than-normal FEV1 reading suggests that you may be experiencing a breathing obstruction. Having trouble breathing is a hallmark symptom of COPD. COPD causes less air to flow into and out of a person’s airways than normal, making breathing difficult.
What could a low FEV1 FVC ratio indicate?
Decreased FEV1/FVC Ratio If your FEV1/FVC ratio is decreased, this is consistent with an obstructive pattern. Damage and/or constriction of the airways is indicative of conditions such as: Asthma. COPD, including chronic bronchitis, emphysema, and bronchiectasis.
Why would FEV1 be low in asthmatic patients?
Obstruction of airflow is defined by a reduced FEV1 (forced exhalation volume in one second) to FVC (forced vital capacity). This is a result in a relatively greater decrease in FEV1 compared to FVC, whereas in restrictive disease these 2 parameters decrease proportionally and the FEV1/FVC ratio does not change.
What is an abnormal FEV1?
Abnormalities of the FEV1 and FEV1/FVC are the result of a decrease in the airflow through the lung, which may be caused by obstructive lung diseases. Examples of obstructive diseases are emphysema and asthma. It is also possible to have situations where both restrictive and obstructive diseases are present.How do you interpret FEV1 results?
The FEV1/FVC ratio is a number that represents the percentage of your lung capacity you’re able to exhale in 1 second. In the absence of restrictive lung disease that causes a normal or elevated FEV1/FVC ratio, the higher the percentage gotten from your FEV1/FVC ratio means the healthier your lungs are.
Is asthma obstructive or restrictive?
Asthma is an obstructive lung condition caused by inflammation of your airways that makes it difficult to breathe. The first step to getting treatment for your asthma is getting a diagnosis.
What is FEV1 in asthma?
Forced expiratory volume (FEV1) is the maximum amount of air you can forcefully exhale in one second. It is used to describe the degree of airway obstruction caused by asthma in a routine test called spirometry or pulmonary function testing, using an instrument called a spirometer.
What FEV1 qualifies for disability?
In order to qualify for benefits, you must meet one of the following requirements: COPD, due to any cause, with a forced expiratory volume one (FEV1) that is equal to or lower to the minimum for your height, between 1.05 for those who are five feet and 1.65 or those who are six feet.What is FEV1 in COPD?
Your FEV1 value is an important part of evaluating chronic obstructive pulmonary disease (COPD) and monitoring progression of the condition. FEV is short for forced expiratory volume. FEV1 is the amount of air you can force from your lungs in one second.
How do you increase FEV1?FEV1 and MVV significantly improved after high-intensity aerobic exercise. In contrast, there were insignificant improvements in FVC. The improvement in FEV1 means that high-intensity aerobic exercise improves air flow in the respiratory tract.
Article first time published onCan allergies cause low FEV1?
Nasal allergy has been demonstrated to be a strong risk factor for the onset of asthma in adults. Spirometric parameters like Forced expiratory volume at timed interval of 1 s (FEV1) and forced expiratory flow (FEF25–75 %) are impaired in patients with nasal allergy or allergic rhinitis.
Is asthma a COPD?
Are COPD and asthma the same thing? No. Chronic obstructive pulmonary disease (also called COPD) and asthma are both diseases of the lungs that make it hard for you to breathe. However, they are different diseases.
What is FEV1 and FVC explain with reference to asthma?
Forced expiratory volume (FEV) measures how much air a person can exhale during a forced breath. The amount of air exhaled may be measured during the first (FEV1), second (FEV2), and/or third seconds (FEV3) of the forced breath. Forced vital capacity (FVC) is the total amount of air exhaled during the FEV test.
How can I test my lung capacity at home?
- Set the pointer. …
- Attach the mouthpiece to the meter. …
- Sit up or stand up as straight as you can, and take a deep breath.
- Close your lips tightly around the mouthpiece. …
- Breathe out as hard and as fast as you can for 1 or 2 seconds. …
- Write down the number on the gauge. …
- Repeat these steps 2 more times.
What should my lung capacity be?
Lung capacity or total lung capacity (TLC) is the volume of air in the lungs upon the maximum effort of inspiration. Among healthy adults, the average lung capacity is about 6 liters.
How can you tell the difference between asthma and COPD on spirometry?
Also, like asthmatics, patients with COPD will have a reduction in their ability to exhale, and will show reductions in airflow when tested with spirometry. However, unlike asthmatic patients, COPD patients will not be able to completely correct their lung function even with treatment.
Does Albuterol increase FEV1?
A positive response to Albuterol was an increase of 9.2% for FEV1 (12% for adults) and 18.5% for FEF25–75.
Does bronchodilator increase FEV1?
Assessing bronchodilator reversibility is important to determine whether fixed airway narrowing is present8. In patients with COPD, post-bronchodilator FEV1/FVC remains < 0.7. However, the FEV1 may improve significantly after bronchodilator, and a change of > 12% AND > 200 mL in FEV1 can occur in COPD1.
What is post-bronchodilator FEV1?
Objective: The GOLD guidelines suggest that the presence of a post-bronchodilator forced expiratory volume in one second (FEV1) < 80% of the predicted value in combination with a FEV1/forced vital capacity (FVC) < 70% confirms the diagnosis of COPD.
Why is it harder to exhale than inhale with asthma?
When things are working normally, the amount of air we breathe in is about the same as the amount of air we breathe out. But during an asthma attack, air gets trapped inside the lungs making it harder and harder to breathe.
What is the life expectancy of someone with restrictive lung disease?
The resulting difficulty in breathing leads to lower levels of oxygen in the bloodstream. In general, the life expectancy with IPF is about three years. When faced with a new diagnosis, it’s natural to have lots of questions.
What happens to FEV1 in restrictive lung?
In restrictive lung disease, both forced expiratory volume in one second (FEV1) and forced vital capacity (FVC) are reduced, however, the decline in FVC is more than that of FEV1, resulting in a higher than 80% FEV1/FVC ratio.
Can FEV1 improve in COPD?
As the disease has a progressive nature, FEV1 usually declines over time [2]. So far, most treatments offer significant symptom improvements, reducing the frequency of exacerbations yet it does not affect the lung function decline, with the exception of smoking cessation [3].
How do you know what stage of COPD you have?
- Stage 1: Mild. At this stage, you may not know you have COPD. …
- Stage 2: Moderate. At this stage, people have a cough, mucus, and shortness of breath. …
- Stage 3: Severe. Your lung function has seriously declined at this stage. …
- Stage 4: Very Severe.
What are the signs of dying from COPD?
- Chest pain due to lung infections or coughing.
- Trouble sleeping, especially when lying flat.
- Foggy thinking because of lack of oxygen.
- Depression and anxiety.
Would a humidifier help with COPD?
Humidifiers, when used correctly, can help maintain the perfect level of moisture in the air (between 30 – 50%), and particularly for COPD patients and anyone with a chronic lung disease, can foster eased breathing, reduced irritation of nasal passages, as well as the ability to more efficiently expel phlegm in …
Can you collect disability if you have COPD?
If you or a loved one has COPD, there may be financial resources available. If your COPD causes you to be out of work for at least 12 months, then yes, you could qualify for Social Security Disability Insurance (SSDI).
Is COPD classed as a terminal illness?
Symptoms of end stage COPD. COPD is terminal. People with COPD who do not die from another condition will usually die from COPD. Until 2011, the Global Initiative for Obstructive Lung Disease assessed the severity and stage of COPD using only forced expiratory volume in 1 second (FEV1).
Can FEV be improved?
Researchers found that FEV 1 increased when healthy individuals replaced 30 minutes per day spent sitting with 30 minutes of any type of physical activity or sleep.
Does exercise increase or decrease your vital lung capacity?
In general regular exercise does not substantially change measures of pulmonary function such as total lung capacity, the volume of air in the lungs after taking the largest breath possible (TLC), and forced vital capacity, the amount of air able to be blown out after taking the largest breath possible (FVC).
Does exercise increase lung function?
How Does Exercise Strengthen the Lungs? When you are physically active, your heart and lungs work harder to supply the additional oxygen your muscles demand. Just like regular exercise makes your muscles stronger, it also makes your lungs and heart stronger.